 
II) Radial shift: This is a relative measurement, which is taken as the difference between the measurements of the fractured radius (c) and the normal, uninjured radius (d). 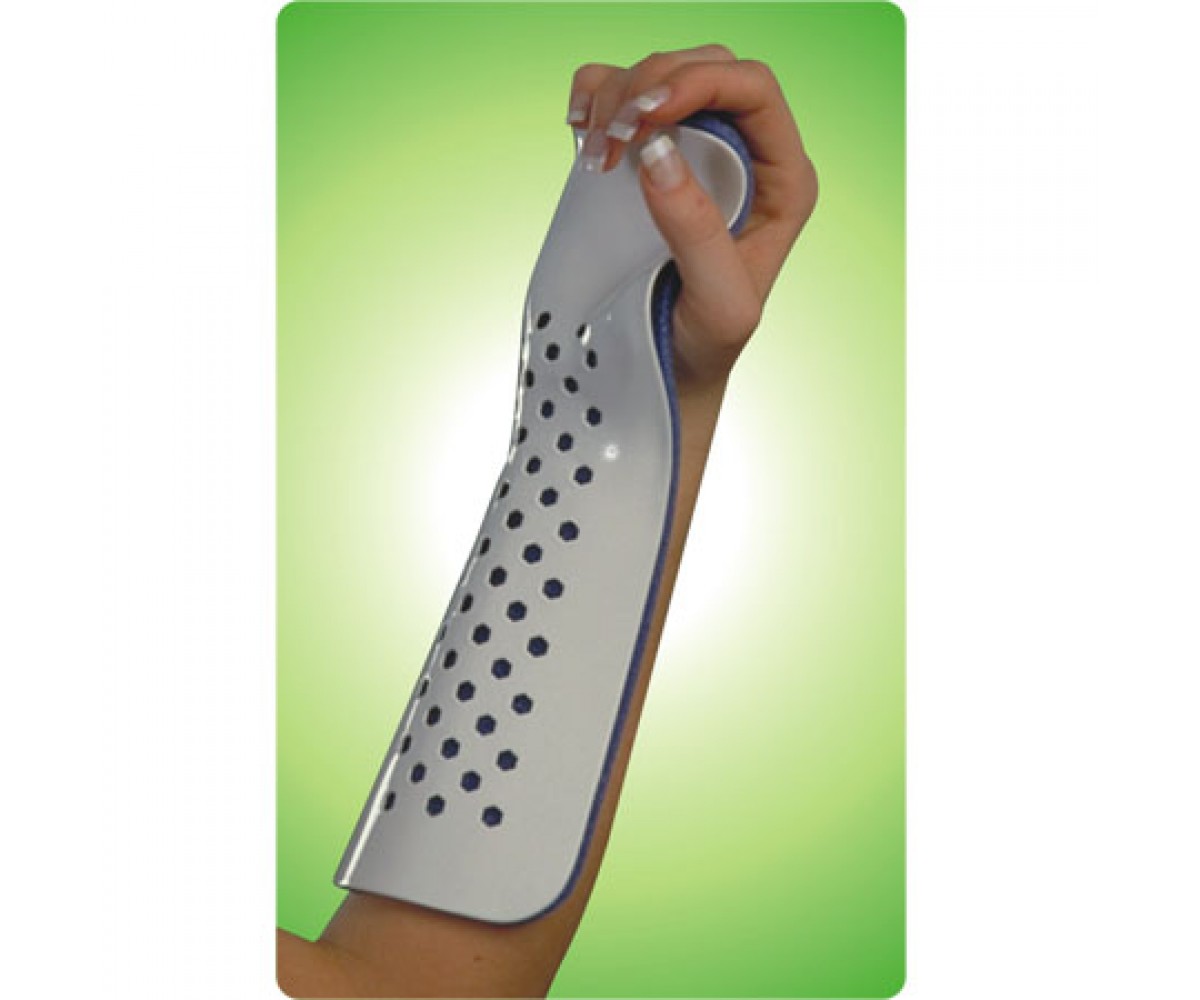
I) Dorsal angulation: The angle between the line which connects the most distal points of the dorsal and volar cortical rims of the radius (a) and the line drawn perpendicular to the longitudinal axis of the radius (b). Radiographic measures of outcome in distal radius fractures. This is a finding that has been observed in many other studies of elderly patients. 15 Interestingly though, there was no correlation between radiographic outcomes and functional outcomes. More than three-quarters of all fractures reverted to a position similar to or worse than the initial deformity.Īnother study of 108 conservatively managed elderly patients (age >65 years) showed better results, with 74% having good or excellent radiographic outcomes. 14 They found no correlation between fracture classification, initial displacement, and final radiographic outcome. 13Ī 2003 study looked at 60 fractures of the distal radius in a low-demand elderly population treated with anatomic reduction and cast immobilization. 12 Similarly, in a prospective study of 50 patients treated with closed reduction and cast immobilization, age was the only statistically significant risk factor in predicting secondary displacement and instability. 11 Age above 60 years was a predictor of failure in a study of 112 conservatively managed fractures as well. 10 A prospective study of 645 Colles’ fractures treated conservatively also found that age was one of the most important predictors of displacement. In a series of ∼4000 distal radius fractures, one of the most significant predictors of instability was increasing age. 9 From radiographic measurements, a significant association of increasing deformity with lower bone mineral density was found.Ī number of studies have looked at predictors of instability in distal radius fractures treated conservatively. In a study involving 125 women aged over 50 years, who suffered distal radius fractures from low-energy trauma, measures of fracture displacement were compared with bone mineral density. Distal radius fractures in elderly people tend to displace because they have osteoporotic bone. This review looks at the current literature related to distal radius fractures in the elderly and the treatment options for stabilization of these fractures.įracture instability refers to the tendency of a fracture to displace after manipulation to an anatomic position. Particularly in the low-demand elderly patient, radiological parameters of adequate reduction do not translate into functional or clinical outcomes (see section ‘Correlation of radiographic outcomes to functional outcomes in elderly patients’). 8įracture displacement in the elderly, however, does not necessarily result in functional impairment. 7 As one would expect, fractures in the elderly therefore tend to displace. 6 Surgical fixation is more difficult because the fixation device cannot gain as robust and reliable hold as in younger, good quality bone. Distal radius fractures in osteoporotic bone have greatly diminished stability there is often bone impaction and fracture fragmentation. The elderly patient, however, presents unique management issues in the treatment of these fractures. These include conservative management with cast immobilization or surgical options: internal fixation, external fixation, percutaneous pinning, and bone substitutes. There are a number of options for stabilization and treatment of these fractures. 4 This conviction, however, has since been proved wrong with complete symptomatic and functional recovery after these fractures being much less than guaranteed. 3 With the growing number of elderly patients in the developed world, the incidence of these fractures will only increase.Ībraham Colles first described the fracture in 1814 stating, ‘One consolation only remains, that the limb will at some remote period again enjoy perfect freedom in all its motions, and be completely exempt from pain the deformity, however, will remain undiminished throughout life’. Eighty-five percent of women who suffer distal radius fractures have been shown to have low bone mineral density and 51% have osteoporosis. 2 In the elderly, they result more commonly from low-energy falls than from high-energy trauma. 1 These fractures have a bimodal age distribution, with young adults and the elderly being the most affected. They are the most common fractures in women in the United States and Northern Europe up to the age of 75 years, with a lifetime risk of ∼15%. They occur more frequently in women than in men. 
Colles’ fractures (fractures of the distal radius) are extremely common. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
